Venous Disease
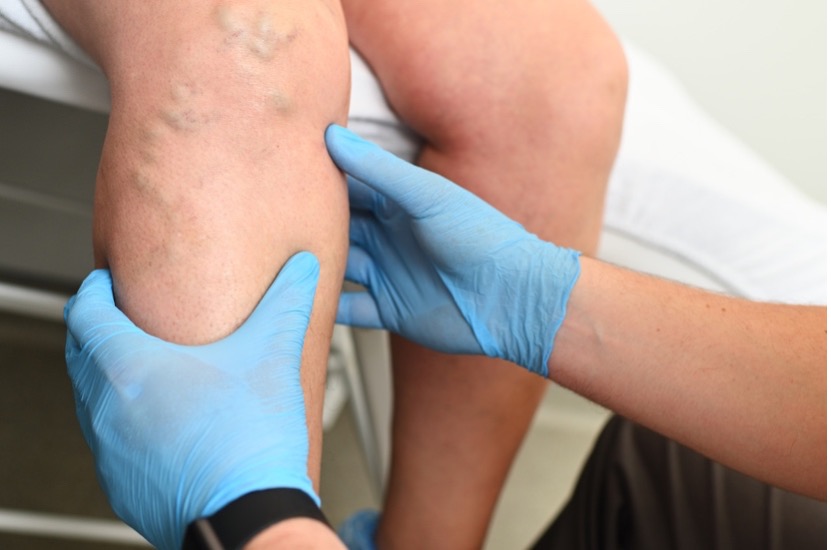
Venous disorders are conditions that damage your veins. Veins are the blood vessels that carry deoxygenated blood from your organs and tissues back to your heart. As people age, problems can develop in the veins that cause a variety of complications. Venous disease of the lower extremities is quite common and affects over 30 million people, but only a fraction seek help. Not only can venous disease lead to ongoing pain and discomfort, but it leads to serious health complications.
At Consulting Cardiologists, we are pleased to have a heart and vascular doctor, Dr. Zain Ahmed, who is both an interventional cardiologist and a vascular interventionalist, on our team. In addition to treating blockages in the heart, he also specializes in treating the veins and arteries outside of the heart, which may cause circulation problems in the legs. Dr. Ahmed has specialized expertise in diagnosing vascular disorders and uses the newest non-invasive treatments to treat a wide range of vascular conditions.
Types of Vein Conditions
There are two primary types of vein conditions—both of which indicate some level of underlying venous insufficiency. Varicose and spider veins are abnormal, dilated blood vessels caused by a weakening in the blood vessel wall.
- Spider veins are tangled groups of tiny blood vessels just under the skin’s surface that resemble spider webs. Typically, they are red, blue, or purple and are clearly visible on the thighs, lower legs, and face.
- Varicose veins tend to be larger in diameter and are visibly bumpy or rope-like. Varicose veins are quite common, though women are affected twice as often as men.
Both types of vein conditions can produce physical symptoms—from leg pain and fatigue to itching, burning, and nighttime restlessness. A comprehensive ultrasound scan can reveal whether the valves in your veins are leaky.
Understanding the Cause
Healthy leg veins have valves that keep blood flowing to the heart. There are several conditions that can interrupt this healthy blood flow.
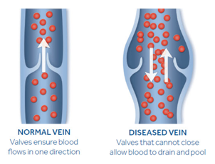
Venous Reflux
This develops when valves stop working properly and allow blood to flow backwards (i.e., reflux) and pool in the lower leg veins.
Chronic Venous Insufficiency
If venous reflux is left untreated, it may worsen over time and develop in a more serious form of vein disease called chronic venous insufficiency (CVI). CVI makes it difficult for blood to return to the heart from the legs. It affects millions of Americans, most over the age of 40. CVI may cause mild symptoms at first. But over time, this condition may interfere with your quality of life and lead to other complications.
Deep Vein Thrombosis
Deep vein thrombosis (DVT) is a blood clot occurring in a deep vein (including upper extremity, arms, and lower extremity, legs). Even though deep vein thrombosis itself is not life-threatening, the blood clot has the potential to break free and travel through the bloodstream, where it can become lodged in the blood vessels of the lung (known as a pulmonary embolism). This can be a life-threatening condition.
Superficial Venous Thrombosis or Phlebitis
Superficial venous thrombosis, or phlebitis, is a blood clot that develops in a vein close to the surface of the skin. These types of blood clots do not usually travel to the lungs unless they move from the superficial system into the deep venous system first. Typically, however, they cause pain.
Ulcers
Ulcers are caused by static blood flow or venous stasis ulcers. Ulcers are wounds or open sores that will not heal or keep returning. Venous stasis ulcers are located below the knee and are primarily found on the inner part of the leg, just above the ankle.
Risk Factors
Family history is a main risk factor for venous disease. For example, if your parents had varicose veins, you have an 89% chance of developing them. Gender also plays a role, women are three times more likely than men to develop venous disease.
Below are additional risk factors for venous disease:
- Age
- Family history of this condition
- Female gender (related to levels of the hormone progesterone)
- History of deep vein thrombosis in the legs
- Obesity
- Pregnancy
- Sitting or standing for long periods
- Tall height
Symptoms of Vein Disease
Symptoms of vein problems vary widely depending on severity. There can be visual signs that you can see just by looking at the legs and feet, and/or there can be a wide range of physical signs.
Visual Signs
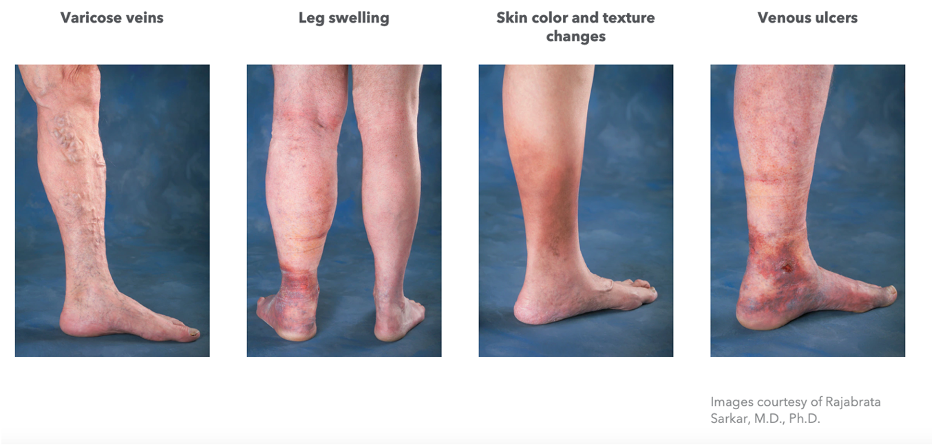
Because vein disease is progressive, vein problems can look very different from person to person. Small veins on the surface of the skin may appear red, blue, or purple (spider veins), while larger veins may become twisted and bulge from the skin (varicose veins).
As vein disease progresses and more veins are affected, the leg may become swollen while the skin becomes firm and discolored due to the insufficient flow and accumulation of blood in the veins. If left untreated, vein disease can lead to open wounds, also known as venous leg ulcers.
Physical Signs
Some individuals only have visual symptoms while others may experience physical symptoms. Ask yourself the following:
- Do you need to sit down, lie down or put your feet up at any point during the day or night because your legs ache and/or swell?
- Do you miss out on parts of your daily routine or doing activities you enjoy because your legs feel heavy, achy, stinging, throbbing, itchy or painful?
- Has anyone in your blood-related family (such as siblings, parents or grandparents) ever had varicose veins or been diagnosed with chronic venous insufficiency (CVI) or leg vein disease?
- Have you experienced any of these symptoms in your legs or ankles? Your symptoms can vary depending on the type of venous disorder and may include:
- Bulging or visible varicose veins
- Leg pain
- Restless legs
- Tired/heavy legs
- Skin color or texture changes
- Tenderness
- Leg cramps
- Red/warm areas
- Aching
- Throbbing
- Itching
- Ulcers/open sores
- Burning/stinging
- Swelling
If you answer yes to any of the above, you may be suffering from vein disease. You are not alone. The good news is this disease is common and treatable!
By the Numbers…
- One in three Americans over the age of 45 has some kind of vein disease.
- Each year, about 1 in 50 adults with varicose veins go on to develop chronic venous insufficiency.
- 41% of women will have varicose veins by age 50.
- 42% of men have some form of venous insufficiency by age 60.
Diagnosing Venous Disorders
If you believe you have symptoms of a venous disorder, the first step is to talk to your cardiologist. Your doctor will ask you to answer some screening questions. If you meet the screening criteria, your doctor may refer you to our specialist, Dr. Ahmed, who has in depth training in vascular disorders.
Dr. Ahmed will start with a complete physical exam and may order lab and diagnostic tests for you to see how well blood is flowing through your veins.
Tests may include:
- Blood tests
- Radiographic imaging such as X-rays, CT scan, and MRI
- Ultrasound
An ultrasound scan is the definitive way to diagnose vein disease and uses sound waves to detect blood clots and observe blood flow in the legs. A technician uses this test to take an image of the inside of the veins in your leg. Dr. Ahmed will review the test results to determine if the valves inside the veins are working properly. He will then determine the source of the issue and the optimal plan for treatment.
Varicose veins and chronic venous insufficiency (CVI) are recognized by many insurance companies, including Medicare and private insurers, as medical conditions.
Treatment Options
The good news is there are many options to address venous disease. This includes newer minimally invasive methods to treat symptomatic superficial venous reflux and varicose veins. The treatments are fast, easy, and painless.
- Treatment is done in the office
- Minimal or no pain
- Same day return to activity
- Typically covered by Medicare and most private insurance companies for cases deemed medically necessary
As seen below, the results can dramatically improve appearance and health.
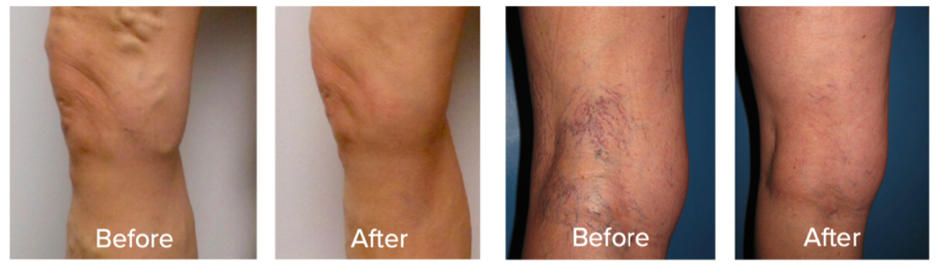
Any patient with persistent lower extremity swelling or visible varicose veins may be a candidate for the newest non-invasive treatment options. This includes post-partum patients. In addition, any patient with chronic non-healing wounds, such as venous stasis ulcers, may benefit from this procedure.
The first step in the evaluation process is a consultation, usually followed by a non-invasive lower extremity ultrasound. It is pain-free and is usually covered by insurance.
Don’t Ignore the Signs
Early symptoms may seem minor. However, they can become more serious if they are not treated. That’s why it is important to be aware of symptoms and seek medical advice at the earliest sign of a problem.
When left untreated, leg vein disease can progress to a condition called chronic venous insufficiency (CVI). If CVI is left untreated, legs can sometimes develop painful sores or wounds on the skin’s surface, called ulcers. Ulcers typically appear near the ankle or lower leg and are brought on from the increased buildup of fluid and blood pressure from veins affected by CVI.
Patients who receive early vein closure treatment along with compression stocking therapy for venous leg ulcers experienced significantly shorter time to healing, and extended time free from ulcers.
Get Started Today!
Our Vascular Center will get you in quickly for an accurate assessment of your vascular health. Call (860) 947-4322 to schedule a consultation.
Meet Dr. Zain Ahmed, Our Vascular Specialist

Dr. Ahmed is an interventional cardiologist who specializes in coronary and peripheral vascular interventions. He did his medical training at the Cleveland Clinic program of Case Western Reserve University, followed by a prestigious medical research fellowship at Harvard Medical School. He completed his internship and residency in Internal Medicine at Brown University in Rhode Island and then completed clinical fellowship training at Yale School of Medicine and Yale New Haven Health. He ultimately completed three cardiology fellowships at Yale in the areas of Cardiovascular Medicine, Advanced Interventional Cardiology–Peripheral Vascular & Endovascular Interventions, and Interventional Cardiology.
As an interventional cardiologist, Dr. Ahmed focuses on diagnosing and treating cardiovascular disease and peripheral vascular disease through catheter-based procedures, such as balloon angioplasty and stenting, in addition to providing general cardiovascular care.
Dr. Ahmed performs vein ablations in our Glastonbury and Wallingford offices.
Celebrating a Milestone
On September 13, 2024, our vascular team performed their 100th vein ablation. Venous ablation is a minimally invasive, outpatient treatment option to treat patients suffering from pain, heaviness, swelling, itching, throbbing, cosmetically unappealing or uncomfortable legs from varicose veins or chronic venous insufficiency.
